Recommended specialists
Article overview
Thyroid surgery - Further information
What’s the thyroid?
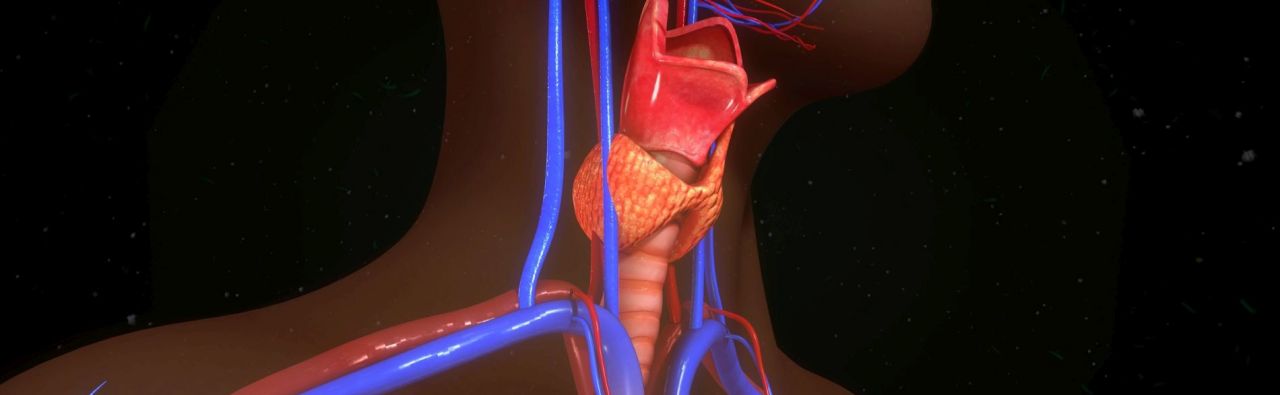
The thyroid gland is an organ that is located in the lower part of the neck and rests on the trachea from the front and the sides. As an important gland its two lobes produce the thyroid hormones triiodothyronine (T3) and thyroxine (T4, tetraiodothyronine) as well as calcitonine. The hormones are involved in complex metabolic processes of the body, such as the regulation of basic metabolism, heart function and blood calcium levels. The production of thyroid hormones is controlled by hormones released from certain parts of the brain.
Closely linked to the thyroid gland are the (usually four) parathyroid glands, which lie against the back wall of the thyroid gland and also produce a hormone, the parathyroid hormone. The parathyroid hormone ensures a constant level of calcium in the blood by removing calcium from the bone if the calcium level is too low.
The entire hormone and metabolic system of the human body is extremely complex and the individual components are finely tuned to each other. If this leads to disorders that can be caused, for example, by an iodine deficiency, the system becomes unbalanced and the thyroid gland may produce too much or too little hormones - with corresponding consequences for the body.
What diseases are treated by specialists in thyroid surgery?
If the thyroid gland is enlarged and produces too much hormone, it is called hyperthyroidism. The patients suffer from increased sensitivity to heat and sweating, diarrhoea, restlessness and insomnia, rapid heartbeat and weight loss. If, on the other hand, the thyroid gland produces too few hormones, this leads to hypothyroidism. Consequences can include reduced performance, fatigue or weakness. The causes of hyperthyroidism or hypothyroidism can be manifold, sometimes requiring only medication, but often also surgical treatment by an expert in thyroid surgery. A goiter, medically called struma, is a visible and palpable enlargement of the thyroid gland.
Basically, the specialists for thyroid surgery distinguish benign thyroid diseases (such as goiter or hyperthyroidism) from malignant thyroid diseases and from thyroid inflammations. The clinical conditions that are treated frequently or in certain situations by thyroid surgery include, for example:
- The euthyroid nodal struma is a benign thyroid disease with enlargement of the thyroid gland and hyperactivity.
- The autonomic nodal goiter, in which the thyroid gland is no longer controlled by the brain, leading to the growth of the thyroid tissue with hyperfunction, is also benign.
- Graves' disease (or autoimmune hyperthyroidism or immunogenic hyperthyroidism) is an autoimmune disease in which the body produces antibodies that stimulate the thyroid gland to increase growth and produce hormones.
- Thyroid autonomy is benign and characterized by hyperactivity.
- Thyroid cancer (thyroid carcinoma) can have its origin in the different cell types of the thyroid gland. Indications of this malignant thyroid disease are usually rapid thyroid growth, hoarseness and/or difficulty breathing.
- Thyroiditis, such as acute thyroiditis, Hashimoto's thyroiditis and Riedel's fibrosating thyroiditis, are only treated surgically in exceptional cases.
- Overactive parathyroid glands (hyperparathyroidism) are associated with increased bone loss and cardiovascular dysfunction. If symptoms occur, the thyroid surgeon will remove all four parathyroid glands.
Which diagnostic methods are used by specialists for thyroid surgery?
The anamnesis (patient survey) is used to inquire about the symptoms of the disease, psychological distress and family predisposition. This can already provide initial indications of a possible therapy. The determination of thyroid hormones in the laboratory is important for functional diagnostics, i.e. for clarifying the question of whether hyper- or hypofunction is present. By palpating the thyroid gland, the doctor can determine whether it has become enlarged, movable or knotty.
With the help of ultrasound examination (sonography), changes such as cysts and nodules can be detected accurately. Occasionally, tissue samples (biopsies, fine needle aspiration) are taken for further examination while using ultrasound. Scintigraphy is often used to determine which areas of the thyroid gland are hyper- and hypofunctional. It can be used, for example, to identify cold knots and hot knots. It plays an important role in the preparation of a thyroid operation.
Occasionally or in the case of certain complaints and suspicion of malignant thyroid diseases, further imaging procedures are used, such as X-ray examination of the chest, possibly using a pap swallow, computed tomography (CT) and magnetic resonance imaging (MRI).
Before a thyroid operation, thyroid surgeons often perform a laryngeal endoscopy to check the functionality of the vocal cords in addition to further laboratory tests (determination of the calcium level in the blood).
Which treatment methods belong to the range of services of a thyroid surgeon?
A surgery will always be necessary if other treatment options (such as medication, isotope irradiation) have not been successful or are not promising. The experts in thyroid surgery will try to completely remove pathologically altered thyroid tissue on the one hand, and to preserve as much functional tissue as possible on the other. This opens up several possibilities for the thyroid surgeon with regard to the quantity of tissue to be removed:
- In lump extirpation, only the diseased tissue, for example a benign tumor (adenoma) or a cold lump, is removed with a margin of normal tissue.
- In lobectomy (hemithyroidectomy), one of the two thyroid lobes is completely removed. This is done, for example, if a local thyroid carcinoma is suspected.
- In the course of the strumaresection, all diseased areas of the thyroid gland are removed, leaving as much healthy tissue as possible, i.e. hormone-producing tissue. The extent depends on the disease and can be more or less extensive.
- In the case of malignant tumors, the thyroid gland is usually completely removed, which is referred to as a total thyroidectomy (complete removal of the thyroid gland).
Depending on the indication, thyroid surgery can be performed as minimally invasive thyroid surgery or as open thyroid surgery. Depending on the amount of thyroid tissue removed, it may be necessary for the patient to consume thyroid hormones after surgery, often including iodine to prevent recurrence.
What distinguishes specialists for thyroid surgery?
First contacts for patients with thyroid diseases are usually specialists for internal medicine and general medicine or also specialists for internal medicine and endocrinology and diabetology. Depending on the thyroid disease, various surgical experts for thyroid surgery may be involved, such as visceral surgeons, oncologists or endocrinologists. For example, visceral surgeons have completed specialist training in visceral surgery and are therefore also specialists for all surgical interventions on endogenous (i.e. inwardly laxative) glands and thus also the thyroid gland. Specialists in thyroid surgery are familiar with both the current and the latest surgical procedures.
Medical spectrum
Therapies
Diseases
References
Literature
Aumüller G, Wennemuth G (2017) Halsorgane. Duale Reihe Anatomie. Thieme, Stuttgart
Dralle H (2012) Schilddrüse. In: Siewert JR, Stein HJ (Hrsg) Chirurgie. 9. Aufl. Springer, Heidelberg
Zünd M, Lüdin M, Lange J (2009) Klinikmanual Chirurgie. Springer, Heidelberg