The abdominal wall is normally stable and consists of several layers of muscle. After abdominal surgery in which stabilizing layers of muscle lying deeper need to be cut through, less elastic incisional tissue develops. This impairs the stability of the abdominal wall at this point, which can lead to the formation of a hernial ring. If a bulge forms in the abdominal wall and if the bowel is able to protrude through etc., this is then called an incisional hernia or rupture.
Recommended specialists
Article overview
- Symptoms of an incisional hernia
- Incisional hernia diagnosis
- Surgical treatment for an incisional hernia
- Surgical techniques in incisional hernia surgery
- Spitzy's surgery
- Techniques with synthetic mesh
- Complications and risks in incisional hernia surgery
- Follow up treatment after incisional hernia surgery
Incisional hernia surgery - Further information
All the factors which impair wound healing after abdominal surgery can lead to incisional hernias. So severe overweight, smoking, metabolic disorders of the connective tissue, several instances of previous abdominal surgery, difficulties with the surgical closure of the abdominal wall, post-operative bleeding and wound infections are all regarded as risk factors for the development of incisional hernias. Because anemia and diabetes can compromise wound healing, patients with these diseases also have an increased risk of an incisional hernia.
Symptoms of an incisional hernia
Although an incisional hernia can cause discomfort, it does not necessarily do so. Initially, the incisional hernia becomes apparent through tension in the scar. Later, this generally becomes recognizable because of swelling and a bulge, which is relatively easy to press back into the abdominal cavity. In the course of time however, especially when standing up or just standing, the incisional hernia can get bigger and become painful, especially when coughing, straining on the toilet or engaging in physical or sporting activities. It can also remain visible when lying down and without straining.
However, if severe pain is suddenly experienced and if the bulge can no longer be pushed back, there is a risk of the protruding bowel becoming trapped. A life-threatening bowel obstruction may be the result. In some circumstances, parts of the bowel will not receive sufficient blood and oxygen. Then the affected area is in danger of dying off, admitting bacteria into the abdominal cavity and the vascular system - all acute risks to life Abdominal pain similar to colic can occur suddenly, with high a temperature, nausea and vomiting.
In such acute cases, the sufferer should go to hospital immediately where incisional hernia surgery will generally be performed as soon as possible. Even if this is not the case, there should be no delay in deciding to have surgery.
Incisional hernia diagnosis
Because of the bulge on the scar and because of other discomfort, the doctor will generally suspect that the patient could have an incisional hernia. The doctor can judge whether and how easily the contents of the hernia sac can be pushed back into the abdominal cavity by feeling the scar.
Depending on the size of the incisional hernia and the weight of the patient, further examinations such as ultrasound, computed tomography or gastrointestinal endoscopy may be necessary in certain cases to enable diagnosis and evaluation of the severity of the incisional hernia. This would reveal the different layers in the abdominal wall and identify any gaps. In this way, for example, the extent of the incisional hernia and risk or even the existence of hernial incarceration can be detected. Further examinations with instruments are normally not necessary. If the hernia can no longer be pushed back, there is a risk of it becoming incarcerated (trapped). At this point, incisional hernia surgery becomes absolutely and immediately essential. But surgery is also necessary if there is persistent discomfort, social withdrawal, reduced quality of life or the likelihood of temporary or permanent incapacity for work.
The time lag after a previous surgical intervention should be at least 3 (but preferably 6) months. After the examination, the patient will be advised on the treatment options and further procedures and also advised on the incisional hernia surgery including the risks.
Surgical treatment for an incisional hernia
A local anesthetic can be administered for the surgery where the incisional hernia is a small one. On the other hand, surgery for a larger incisional hernia with a wider opening of the abdominal cavity will be performed under a general anesthetic. An anesthetist explains the administration and risks of the anesthetic before surgery takes place. For incisional hernia surgery under a general anesthetic, plans should be made for in-patient admission of about 5 to 10 days in a hernia center, depending on post-surgery developments. On the day before the surgery, the patient will be given a mild laxative and anti-thrombosis treatment and a sedative on the day of the incisional hernia surgery itself.
Surgical techniques in incisional hernia surgery
Depending on the type of the original abdominal surgery and the size of the rupture, the hernial gap is treated by means of abdominal incision as open incisional hernia surgery or by the minimally invasive abdominal endoscopy technique (keyhole surgery) as closed incisional hernia surgery. The standard procedure is open incisional hernia closure with synthetic mesh as reinforcement.
In closed hernia surgery, access to the hernial ring is gained through the abdominal wall by means of abdominal endoscopy (laparoscopy). Through this technique, the abdominal cavity and the organs located in it become visible and the hernial ring can be closed directly with special instruments and additionally a synthetic mesh can be attached to the abdominal wall. For patients, laparoscopic incisional hernia surgery is a pleasant and gentle technique. Post-operative pain is reduced, the incidence of wound infection is significantly lower and patients quickly regain their ability to take physical strain.
In open incisional hernia surgery, the hernia sac is exposed by an incision and the contents of the hernia sac are pushed back into the abdominal cavity. The hernial ring can be closed by means of directly suturing the fascia (supporting fibrous layers in the abdominal wall), by means of doubling the fascia or by stabilizing the hernial ring closure with synthetic materials. In fascia doubling, the edges of the abdominal wall layers (fascia) are overlapped or doubled for suturing, which creates greater stability. This incisional hernia surgery is also called Mayo hernia repair. In larger incisional hernias, the suture is generally reinforced with insoluble synthetic mesh or a combination of synthetic mesh and material from the patient's body.
Spitzy's surgery
In a small incisional hernia (hernial ring < 2 cm) closure is effected by suturing the edges of the rupture with a robust suture. Although this surgery is performed under general anesthetic, it is generally on an out-patient basis. The particular advantages of this technique are the short performance time, the low-level trauma and the very minor incidence of complications. Because the technique does not include reinforcement with synthetic mesh there is the increased risk of a secondary rupture. Also, the patient must take it easy physically for several weeks until healing is complete.
Techniques with synthetic mesh
Used in both closed and open surgery, the synthetic mesh is usually made of polypropylene, which is very well tolerated. However, because the mesh does not come into direct contact with the bowel loops (risk of adhesions), for some years there have been polypropylene meshes with a layer that prevents adhesions.
The difference between the different incisional hernia surgical techniques with synthetic mesh lies in the position of the mesh within the abdominal wall. The commonest techniques for incisional hernia surgery are the sublay technique (below the abdominal muscles) and the intraperitoneal onlay mesh technique (IPOM, position of the mesh between the bowel and peritoneum). In addition, there is also the inlay technique in which the mesh is positioned in the hernia gap.
Incisional hernia surgery: IPOM technique (intraperitoneal onlay mesh)
In this technique, the abdominal cavity is first filled with gas (pneumoperitoneum) and then any adhesions present are removed (adhesiolysis).
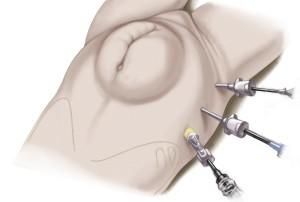
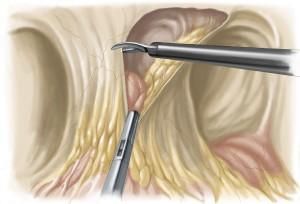
A synthetic mesh fixed to the interior of the abdominal wall, between the bowel and peritoneum, covers the hernia gap from inside.
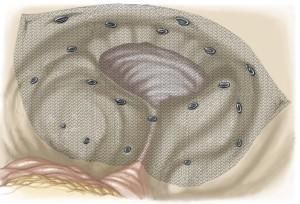
Because this incisional hernia surgery is generally performed with keyhole surgery, the incidence of wound infections and post-operative pain is very low. However, large ruptures cannot always be treated with this technique.
Sublay mesh
The sublay mesh technique is an open surgical procedure for large incisional hernias, which are only performed under general anesthetic. In this, an incision is made in the skin above the hernia sac and the hernia sac is exposed and where applicable removed.
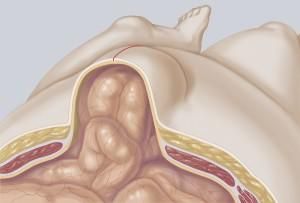
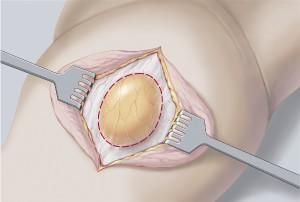
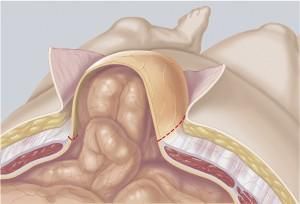
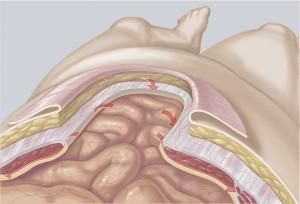
Any adhesions in the abdominal cavity are detached and the contents of the hernia sac are pushed back into the abdominal cavity. The synthetic mesh is fixed below the abdominal muscles with a few sutures or a fibrin adhesive.
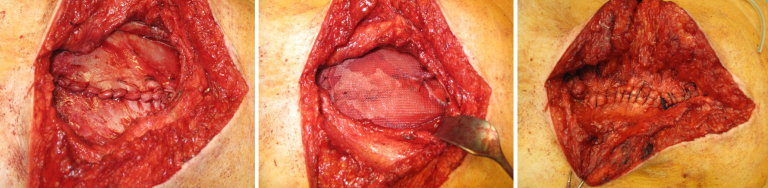
Complications and risks in incisional hernia surgery
The following may occur after incisional hernia surgery - wound infections, seroma production (accumulations of body fluids in cavities in the wound area) and hematoma (bruising). Mesh usage entails an infection rate of up to 10%. On the other hand, hematoma and seroma production are significantly more frequent when mesh is used then after direct closure of an incisional hernia. The fluid accumulation disappears after roughly 2 to 6 weeks. Large accumulations of fluid can be removed by puncturing the site.
Calluses can form near the surgery site and damage to nerves can result in a generally temporary, and rarely long-lasting feeling of numbness. Occasionally, patients also complain of being restricted in their movements and also of pain around the abdomen. However, the likelihood of a secondary hernia is not uncommon even when modern synthetic meshes are used.
Follow up treatment after incisional hernia surgery
Patients can continue to eat as normal after incisional hernia surgery, depending on the repaired incisional hernia. Where applicable, a return to a normal diet can be step by step and the outcome of the incisional hernia surgery is monitored by ultrasound. Directly after surgery, an elastic support garment is often fitted to provide support. This should be worn for several weeks both day and night. After the suture threads have been removed, 10 to 12 days post-surgery, physical exertion can be gradually resumed although heavy physical effort (lifting weights of more than 20 kg) should be avoided for up to 3 months, depending on the incisional hernia and associated treatment technique. However, no special aftercare is needed.
























