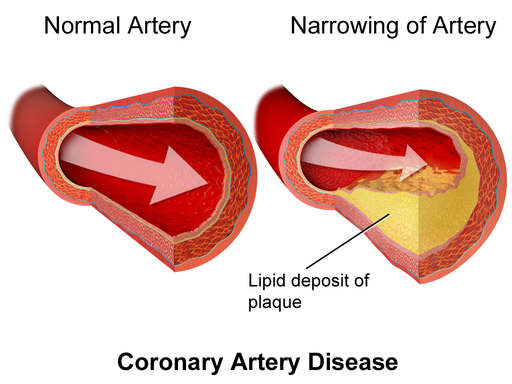
Coronary heart disease (CHD), also known as coronary artery disease (CAD), is a disease in which fatty substances called plaque build up on the walls of your coronary arteries. These are the arteries that deliver oxygen-rich blood to your heart muscle.
The build-up of plaque can cause a narrowing of the arteries. This in turn can reduce the oxygen supplied to your heart. When this occurs, you may experience angina (chest pain), and there is also a risk you could suffer a heart attack, which is a serious health problem.
When the blood supply to your heart is reduced, you may experience a number of symptoms. The most common of these is chest discomfort (angina). Some people describe this as:
- chest pain
- tightness
- a heavy feeling
- burning or squeezing sensations
Similar symptoms can occur with indigestion and heartburn.
Further symptoms of coronary heart disease may include:
- pain in your arms, or in your left shoulder
- breathlessness
- dizziness and sweating
Usually, the more restricted your blood flow, the more symptoms you are likely to experience. A complete blockage could even prevent your blood flowing and result in a heart attack, requiring immediate medical treatment.
Though females can experience all of the above-mentioned symptoms, they are also more prone to:
- nausea and vomiting
- back pain
- jaw pain
- breathlessness, but without any sign of chest pain
Reduced blood flow may also cause anyone’s heart to:
- become weaker
- develop cardiac arrhythmia (irregular heart rhythms)
- pump insufficient blood for their bodily needs
Arteriosclerosis (plaque build-up within the arteries) is the most common cause of coronary heart disease. This gradually hardening plaque material effectively narrows one or more of the coronary arteries, which results in reduced blood flow and/or a blockage.
Plaque may also rupture or break open and release platelets (blood cell fragments) into your bloodstream. These may collect together and form blood clots, which can also cause a blockage in a coronary artery and lead to a heart attack.
Diagnosis begins with a physical examination alongside a review of your medical history. There will also be some other tests, which may include:
- an electrocardiogram to monitor your heart’s electrical signals and check for a possible heart attack
- an echocardiogram to create an image of your heart and check its function and performance
- a stress test to check your blood flow while you are active and at rest
- a cardiac catheterization procedure, which uses dye to reveal the detail of your coronary arteries
- a heart CT scan, which uses X-rays and can reveal the presence of any calcium deposits inside your arteries
When coronary heart disease is diagnosed, the aim wherever possible is to lower risk factors and use treatments to reduce the likelihood of a heart attack or stroke. The treatment options chosen will always depend on your state of health and the risk factors present, as well as on your general physical condition. One strategy your doctor may adopt is to prescribe medication – for example, to address high blood pressure or diabetes.
To further reduce your risk factors, some lifestyle changes may also be recommended, such as:
- losing weight
- exercising regularly
- giving up smoking
- reducing your alcohol intake
- switching to a healthier low-fat, low-sodium diet
Where medication and lifestyle changes are unable to effect sufficient improvement, there may be a need to improve the blood flow to your heart by one of the following medical procedures:
- a coronary bypass, which surgically attaches a new piece of healthy artery to allow blood to flow around a blocked or damaged coronary artery
- an angioplasty procedure, which uses a small inflatable balloon to widen a blocked artery and remove any plaque build-up, plus a wire mesh support to prevent any subsequent narrowing
- a non-invasive, enhanced external counter pulsation procedure, which stimulates the development of fresh blood vessels around the location of blocked arteries
The outlook for those with coronary heart disease will vary from person to person. Your chances of recovery will be enhanced by starting treatment and/or making lifestyle changes as soon as possible.
Prevention of CHD involves controlling your risk factors, as advised by your doctor. There are only a small number of risks (for example, family history, age and gender) that cannot be addressed by such means.




















