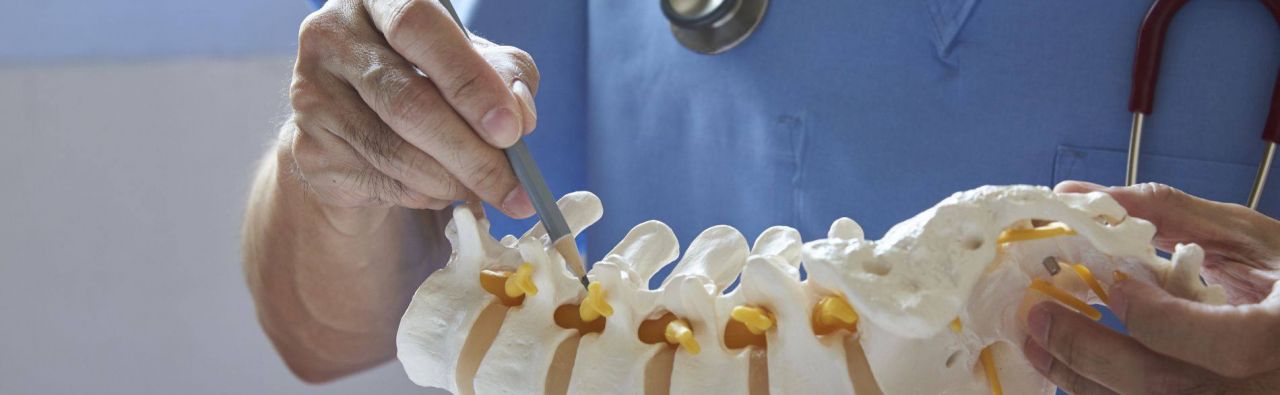
Spinal disk endoprosthetics is the insertion of a new, artificial disk, a so-called disk prosthesis. This spinal disk replacement is intended to eliminate the pain caused by the disk on the on hand and to maintain the mobility of the spinal column on the other hand.
Recommended specialists
Article overview
- What is spinal disk endoprosthetics?
- Which diseases are treated by specialists for spinal disk endoprosthetics?
- Which diagnostic methods are used by specialists for spinal disk endoprosthetics?
- Which treatment methods belong to the range of services of a specialist for spinal disk endoprosthetics?
- What distinguishes specialists in spinal disk endprosthetics?
- References
Intervertebral disk endoprosthetics - Further information
What is spinal disk endoprosthetics?
The human spine consists of 24 vertebrae, which in turn consist of a compact vertebral body and a hole formed by the vertebral arches. Thereby, the vertebral canal (nerve canal) is created, in which the spinal cord, a part of the nervous system, runs. Between the vertebral arches, the spinal cord nerves (spinal nerves) emerge from the spinal canal. As a kind of shock absorber, the spinal disks connect two vertebral bodies with each other. This is why the spinal disk is also known as the intervertebral disk. It consists of an outer fibrous ring and a gelatinous core located in the center. In particular, the gelatinous core is responsible for absorbing shocks to the spinal column. In the course of life and under constant strain, the water content in the gelatinous core decreases, the intervertebral disks become thinner and pathological changes (wear) to the bones of the vertebral bodies can occur. Small cracks in the fibrous ring can cause the gelatinous nucleus to pass through the fibrous ring to the outside - resulting in a herniated disk. This can then press on the spinal nerves or the spinal cord and cause severe pain and neurological deficits.
A disk prosthesis consists of two metal plates to be attached to the vertebral bodies and a movable plastic core. They are typically inserted from the front, i.e. through the neck or abdominal cavity.
Which diseases are treated by specialists for spinal disk endoprosthetics?
The main reason for the implantation of spinal disk endoprostheses is pain and/or neurological deficits as a result of degenerative (wear-related) changes, i.e. wear and tear of the spinal disk or vertebral bodies due to age, strain or illness.
In a herniated disk, the pressure on the nerves is relieved by removing the disk material and the correct distance between the vertebral bodies is restored by inserting a disk prosthesis. As a rule, the mobility of the vertebrae is maintained.
In spondylosis, the vertebral bodies undergo degenerative changes as a result of constant incorrect strain and overweight. New bony structures are formed which either exert pressure on the spinal nerves or over time can contribute to stiffening of the spinal column. Before the disk prosthesis is inserted, the bony neoplasms are removed.
If the intervertebral disk and adjacent bone structures are degeneratively altered, osteochondrosis is present.
Slight forms of myelopathy (spinal cord damage), which result from a narrowing of the spinal canal (spinal stenosis), can also be treated by a specialist in intervertebral disk endoprosthetics. Non-specific back pain can also be an indication for an artificial spine disk, if the cause of the pain is related to the intervertebral disk.
Which diagnostic methods are used by specialists for spinal disk endoprosthetics?
In many cases, the patient's medical history and a physical and clinical examination can be used to determine the possible causes of the patient's complaints. Imaging procedures in particular enable experts in spinal disk endoprosthetics to gain an accurate picture of the spine, vertebrae and intervertebral disks as well as the spinal canal and spinal cord.
X-rays of the spine can be used to visualize it, detect changes in the vertebral bodies (such as spondylosis) and assess the intervertebral spaces. It can also be used to take functional images to check stability and mobility. Magnetic resonance imaging (MRI) or computed tomography (CT) can be used to assess the intervertebral disks and the spinal canal and identify possible herniated disks.
Myelography, i.e. the injection of a contrast agent into the spinal canal in order to better visualize the spinal cord and spinal nerves, is only used in rare cases. Prior to a possible disk prosthesis operation, a contrast agent may be injected directly into the disk space (discography) and its spreading may be made visible in the X-ray image. Depending on the distribution of the contrast agent, conclusions can be drawn about the type of disk damage.
Which treatment methods belong to the range of services of a specialist for spinal disk endoprosthetics?
The range of services of a specialist for spinal disk endoprosthetics includes the following methods:
- Removal of a herniated disk in the area of the cervical spine and lumbar spine and the insertion of an artificial disk.
- Treatment of osteochondrosis by implantation of an intervertebral disk prosthesis
- Removal of bone regeneration in spondylosis and insertion of an intervertebral disk prosthesis
- Decompression surgery (relief surgery) in spinal canal stenosis by removal of the constricting bones and ligament structures
What distinguishes specialists in spinal disk endprosthetics?
Experts in intervertebral disk endoprosthetics are usually specialists in orthopedics and trauma surgery or specialists in neurosurgery who have special experience in the field of implanting spinal disk prostheses. When deciding for or against a surgery, they weigh up the opportunities and risks against each other and consider possible alternatives for an endoprosthesis. Through certification, they guarantee high quality in surgical care.
References
- Bundesärztekammer (BÄK), Kassenärztliche Bundesvereinigung (KBV), Arbeitsgemeinschaft der Wissenschaftlichen Medizinischen Fachgesellschaften (AWMF) (2017) Nationale VersorgungsLeitlinie Nicht-spezifischer Kreuzschmerz – Langfassung, 2. Auflage. Version 1
- Gravius S, Weißkopf M, Ohnsorge JAK (2007) Die lumbale Bandscheibenprothese: Eine narrative Übersicht. Dtsch Arztebl 104(38): A-2592 / B-2290 / C-2222
- Ogon M, Meissner J, Tuschel A et al. (2006) Die Bandscheibenprothese an der Halswirbelsäule. J Miner Stoffwechs 13(1):14–17
- Schünke M et al. (2018) Prometheus. Allgemeine Anatomie und Bewegungssystem: LernAtlas der Anatomie. Thieme, Stuttgart
- Zechmeister I, Winkler R (2010) Bandscheibenprothesen: Systematischer Review. Decision Support Dokument Nr. 38. Ludwig Boltzmann Institut