A blood vessel is basically a tube through which blood flows. It is formed by the vessel wall. The wall of larger blood vessels consists of three layers of tissue lying on top of each other:
- inner vascular layer (intima),
- middle vascular layer (media) and
- outer vascular layer (adventitia)
The cavity inside a vessel is called the lumen.
Splitting of the vessel wall layers occurs when the inner layer tears but the outer layer remains intact. Then blood from the lumen enters through the tear into the space between the two layers.
Due to the increased pressure in the aorta more and more blood enters the intermediate layer. This causes the layers to diverge over long distances and can form an unnatural gap. This allows the actual lumen to be completely closed.
The intima usually cannot withstand the high pressure and tears again at another point. This allows the blood to flow back into the aorta.
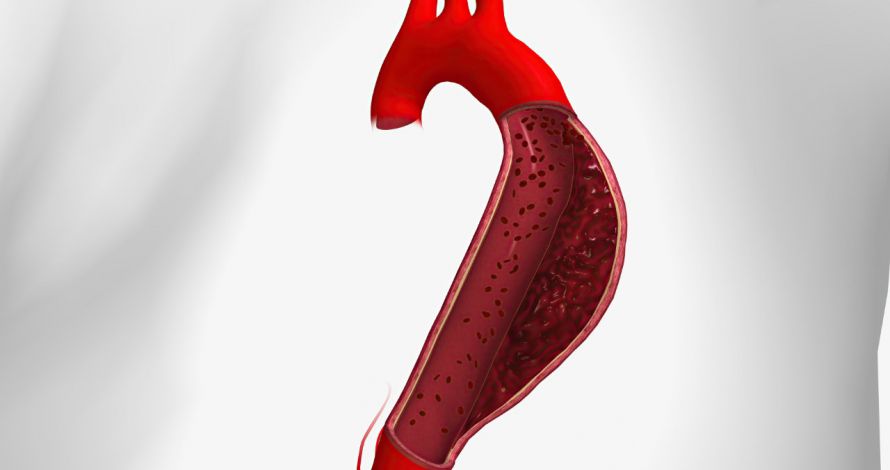
Illustration of an aortic dissection with blood in the interspace of the aortic vessel wall © htcmed | AdobeStock
The following are considered risk factors for the development of aortic dissection arteriosclerosis and structural weakness of the media (mediadegeneration). Such a structural weakness is often seen in patients with congenital heart valve anomalies or connective tissue diseases. Corresponding diseases are, for example, Marfan syndrome or Ehlers-Danlos syndrome.
Other risk factors are an older age as well as high blood pressure. In addition, traumatic events can be the cause of an aortic dissection, such as an injury to the vessel wall during a catheter examination.
The signs of the disease depend on the location and extent of the dissection. Some patients with chronic aortic dissection have no symptoms at all. In others, sudden cardiac death can occur in extreme cases when the aorta ruptures.
Typically, an acute aortic dissection manifests itself by a sudden, sharp, stabbing or tearing pain in the chest. It can radiate to the shoulder blades and back.
Depending on the affected section of the vessel, other symptoms may occur, such as
The blood loss may cause symptoms of shock, such as
- Accelerated pulse,
- Drop in blood pressure,
- Impaired consciousness.
Depending on the location of the tear and the extent of the bleeding, several categories can be distinguished. The DeBakey classification defines three types of aortic dissection:
- DeBakey I: Tear in the area of the ascending aorta (aorta ascendens), the bleeding extends beyond the aortic arch.
- DeBakey II: Rupture also in the ascending aorta, but re-entry of bleeding still occurs in the ascending aorta.
- DeBakey III: Entry and re-entry are in the descending aorta.
A further development is the Stanford Classification. It distinguishes only two types based on the localisation of the entry:
- Stanford A (= DeBakey I and II): Tear in the ascending aorta,
- Stanford B (= DeBakey III): Tear in the descending aorta.
The location of the tear is decisive for the patient's risk and thus for the treatment. Therefore, aortic dissection specialists mainly use the Stanford types to assess the disease.
If an aortic dissection is suspected, imaging can show bleeding in the aorta. First indications can be
- the X-ray image of the thorax with its organs and
- the ultrasound examination (Sonography) of the abdominal cavity
The transesophageal echocardiography (TEE, ultrasound examination via the oesophagus) enables a precise assessment of the aorta near the heart and the descending aorta.
Doppler technology also allows differentiation of the normal and "false" lumen, entry and re-entry can usually be detected. Contrast-enhanced computer tomography (CT) provides good visualisation of the extent and relationship of the aortic dissection to the adjacent vessels. Magnetic resonance imaging (MRI) is also a reliable method for diagnosing aortic dissection. Angiography (method of imaging the vessels) can also provide important insights.
The location of the tear is decisive for the treatment.
An acute Stanford A-type dissection must be considered an emergency and should be operated on as soon as possible. The affected section of the vessel is usually removed and replaced by a vascular prosthesis.
The implantation of vascular prostheses in the aorta means a relatively high risk for the patient. That is why a Stanford B type dissection is initially treated with a wait-and-see approach. This means that the doctor observes the development of the dissection. Only when the situation deteriorates, for example in the case of
- threatened occlusion of vascular outlets,
- rapidly increasing vessel diameter or
- threatened rupture of the aorta,
is treatment initiated.
Complications such as blocked vessel outlets are treated by aortic dissection specialists using catheters. By means of Stent implantation the vessel wall can be stabilised and, if necessary, an artificial re-entry can be created. This reduces the pressure in the "false lumen" and thus reduces the risk of rupture.
The treatment of the pain and the lowering of the blood pressure is carried out using medication.















