Cerebral hemorrhage is also referred to as a brain hemorrhage or intracranial hemorrhage. The latter term refers to the cranium, the Latin word for skull. This refers to all bleeding within the skull.
The effects on the brain and the resulting symptoms also depend on the extent and location of the bleeding. Medical professionals classify hemorrhages by the name of the delimiting meninges (membranes):
- Epidural hemorrhage (epidural hematoma, EDH): Bleeding between the skull and the hard meninges (dura mater)
- Subdural hematoma, SDH: Hemorrhage directly under the hard meninges while being over the soft meninges
- Subarachnoid hemorrhage, SAH: Bleeding below the arachnoid mater (soft meninges).
- Intracerebral hemorrhage, ICH: Hemorrhages in the brain substance
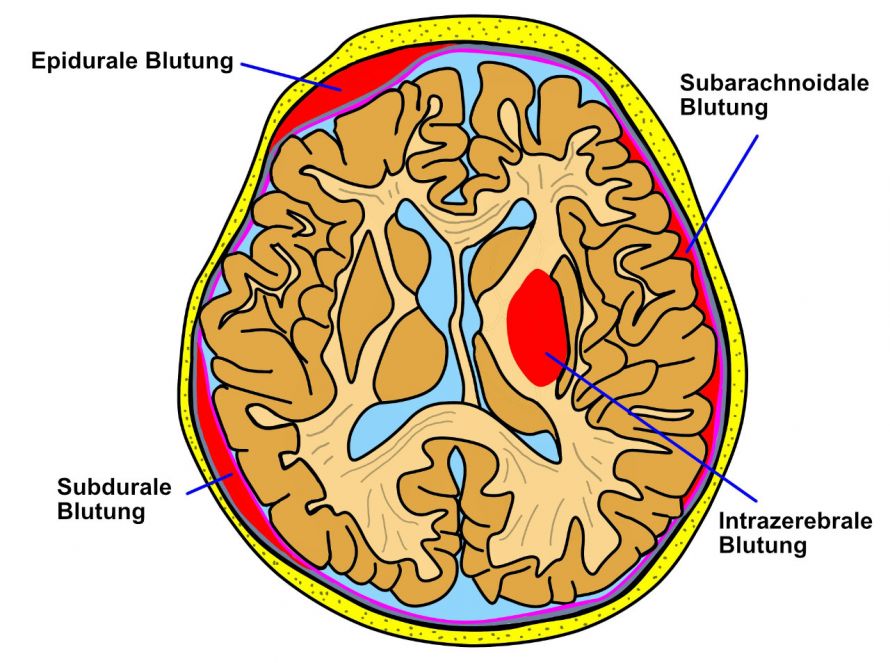
Brain hemorrhages are named based on the meninges adjacent to them © songkram | AdobeStock
All four of the above types of cerebral hemorrhage can occur as a result of trauma. Intracranial hemorrhages in the area of the meninges (epidural hematoma and subdural hematoma) are particularly common as a result of head trauma. This includes
- Traffic, sports, and work accidents,
- Violent crime involving blows or knocks to the head.
Intracerebral hemorrhage
Hypertension is the most common trigger of intracerebral hemorrhages. Elevated blood pressure levels over a prolonged period of time damage the blood vessels. This can cause them to rupture, triggering a brain hemorrhage.
Other risk factors that increase the likelihood of developing a cerebral hemorrhage include:
- Advanced age,
- Smoking tobacco,
- Excessive alcohol consumption,
- The use of hard drugs,
- A high blood lipid level,
- Lack of movement,
- Brain tumors, and
- Vascular malformations.
An intracerebral hemorrhage presents with signs of disease similar to those seen in a stroke. This results from a circulatory disorder. The symptoms are
Loss of consciousness is also possible.
Subarachnoid hemorrhage
Head trauma often leaves a more or less pronounced subarachnoid hemorrhage. In some cases, however, a ruptured aneurysm is responsible for this type of bleeding.
An aneurysm is a sac-shaped bulging of a blood vessel (arterial or venous). It results from a local weakness of the vessel wall in the area of an arterial vessel branching in connection with
In the case of a subarachnoid hemorrhage, a particularly intense headache occurs suddenly. It is accompanied by neck pain or a stiff neck.
The symptoms usually begin during intense physical exertion. Other symptoms are
- Nausea,
- Vomiting,
- Impaired consciousness.
Subdural hemorrhage
Two types of subdural hematomas can occur:
- Acute as a recent hemorrhage
- Chronic as a hemorrhage that has existed for a longer period of time.
Chronic subdural hematomas mainly affect the elderly. The cause is the dwindling brain volume and the resulting increasing strain on the bridging veins. Chronic subdural hematomas develop slowly over several weeks.
Most often, a mini-trauma to the head is the trigger; in some cases, there was no relevant trauma at all. Blood-thinning medications increase the risk of chronic subdural hematomas.
Chronic subdural hematomas may persist for a long time without clinical symptoms. Possible symptoms are
- Headaches,
- A feeling of pressure in the head,
- Dizziness, and
- Newly occurring cognitive changes.
Focal neurological deficits or instances of impaired consciousness are also possible.
Acute subdural hematomas usually result from a more severe accident in which blood vessels in the subdural space are damaged.
The clinical symptoms of an acute subdural hematoma include
Specific symptoms are
These are particularly observed when there is pressure on the brain. These deficits are very similar to the symptoms of epidural hematomas.
Epidural hemorrhage
The most common cause of epidural hemorrhage is a skull fracture resulting in injury to an artery of the dura mater. Very often an accident is the trigger. The spread of the hematoma occurs only within the cranial sutures.
An epidural hemorrhage is most commonly associated with loss of consciousness immediately following trauma.
Rather rarely, but characteristically, the patient may reawaken after head trauma and be relatively symptom-free for a few minutes. This is called a free interval. A little later, the following symptoms typically occur
- Headaches,
- Nausea,
- Vomiting, and
- Neurological dysfunctions with subsequent impairment of consciousness.
The effects of a brain hemorrhage can be fatal. That is why swift action is necessary. The later the patient is treated, the more likely the cerebral hemorrhage can lead to death.
The emergency doctor should therefore be made aware of even the slightest suspicion!
A CT (computed tomography) scan of the head provides information about where the bleeding is located. A hospital with a neurosurgical department should be consulted for further treatment.
There is always a risk of brain swelling with a cerebral hemorrhage. The resulting increase in intracranial pressure affects the entire body. The result is an undersupply of the brain. Various measures, i.e.,
- Artificial respiration,
- Lowering of blood pressure through medication, and
- Diuretic infusions
are the first treatment steps taken to counteract this. With these steps or also external cerebrospinal fluid drainage, the volume of cerebrospinal fluid and thus the intracranial pressure can be regulated.
Major hemorrhages cause extreme intracranial pressure and are therefore usually surgically removed.
In the course of the operation, the surgeon opens the skull in the affected area. There, the surgeon removes the bruise and stops the cause of bleeding.
Despite rapid treatment, patients can still die in some cases.
Thus, all intracranial hemorrhages are serious illnesses. They require emergency treatment.
Different types of neurological damage occur depending on the location of the brain hemorrhage. Hemiparesis symptomatology with decreased sensory perception and strength on one side of the body is particularly common. Some sufferers experience only mild gait unsteadiness. Others, however, struggle with extensive paralysis.
Incomplete hemiplegia affects the face as well as the arms and legs.
As further consequences,
- Impaired coordination of movements (ataxia),
- Problems with more complex movements (apraxia), and
- A decreased awareness in one-half of the body
can occur.
Rapid treatment in the hospital is usually followed by a period of neurological rehabilitation. It is used to improve the chances of success after emergency treatment.
The various areas affected such as
- Language,
- Sight,
- Concentration, and
- Movement
require good cooperation between therapists from different medical specialties:
- Occupational therapy,
- Physiotherapy
- Physical therapy,
- Speech therapy,
- Neuropsychology, and
- Case management (social services)
The prognosis for recovery depends on the size and spread of the hemorrhage, among other factors. The patient's state of consciousness upon admission to the hospital is also important.
Some of those affected recover fully after the brain hemorrhage. However, the majority of those affected can only partially master their daily lives on their own, or only after several months or years.


















