Recommended specialists
Article overview
- What is knee endoprosthetics?
- Which disorders are treated by knee endoprosthesis specialists?
- Which diagnostic techniques do knee endoprosthesis specialists use?
- What treatment techniques are included in the range of services performed by knee endoprosthesis specialists?
- What are the special features of knee endoprosthesis specialists?
- References
Knee endoprosthetics - Further information
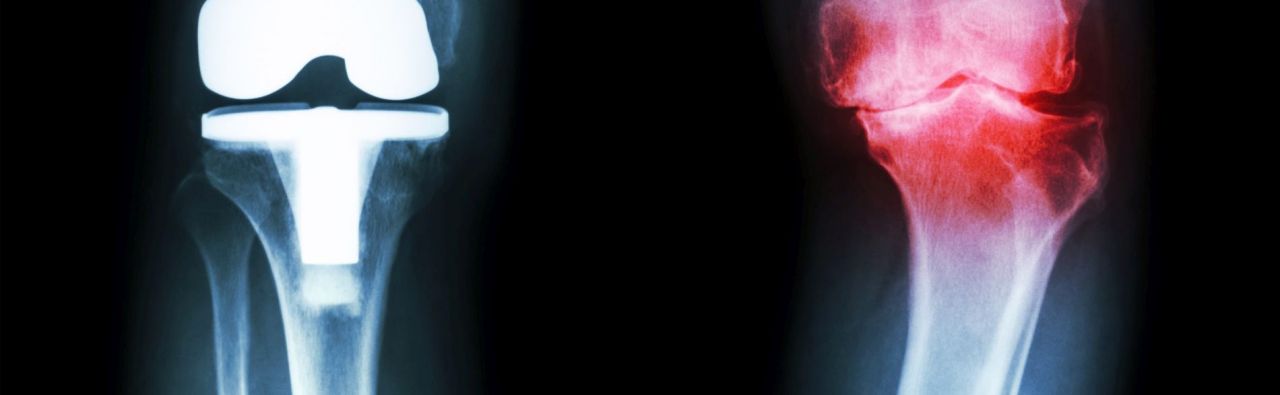
What is knee endoprosthetics?
The human knee joint consists of a femur (thigh bone) and a tibia (shinbone) and the patella (knee cap). These bones are connected to each other by means of sinews and ligaments (cruciate ligaments, lateral collateral and medial collateral ligaments, quadriceps sinew and patellar ligament) and so give the knee joint the necessary stability. The areas of the femur and tibia involved in the knee joint are contained in the joint capsule, which is filled with joint fluid. The joint fluid (synovia) acts as a source of nutriment for the layers of cartilage present on the bone. On the one hand, it prevents direct contact between bones and on the other, together with the two menisci (pieces of rubbery cartilage), acts as a kind of shock absorber to cushion against impacts.
Because the human knee has such a complex structure and because of the special mechanical demands made on an artificial knee joint, the implantation of an artificial joint into the knee is a very complex procedure.
Which disorders are treated by knee endoprosthesis specialists?
Rheumatic diseases (for example inflammation of the joints, known as rheumatoid arthritis), severe overweight, malpositions (knock knees, bow legs), deformations or injuries (post-traumatic arthritis) can initially destroy cartilage and then the bone areas involved in the joint. This process is known as arthrosis, i.e. an excessive degree of osteoarthritis (joint wear). If arthrosis occurs in the knee, this is termed gonarthrosis. It is always when the osteoarthritis is so far advanced that conservative therapies or surgical interventions to maintain the joint are no longer beneficial that a joint replacement is considered.
The stability of the knee joint can be so severely compromised by injuries to the ligaments that here, too, a knee joint prosthesis becomes necessary. Also, bone tumors or comminuted fractures (bone fractures) can make it necessary to implant a knee endoprosthesis.
Which diagnostic techniques do knee endoprosthesis specialists use?
If discomfort and anamnesis (patient survey) indicate a suspected arthrosis or some other change or disorder of the knee joint, an X-ray examination can be a very good means of determining the condition of the bones. In addition to this, magnetic resonance tomography (MRT) can be used to reveal the state of joint cartilage and ligaments. An ultrasound examination (sonography) also reveals the soft tissue and the fluid-filled cavities (joint capsules). In rare cases, bone scintigraphy can be used for a more precise examination of bone area located beneath the cartilage. Depending where and to what extent enrichment occurs after administration of a substance, conclusions can be drawn about the degree of cartilage degradation and any early stage bone impairment. However, this technique is actually no longer in current use.
To enable the use of specially constructed prostheses, computed tomography is used to determine the exact anatomical dimensions before knee joint surgery. The computer then models a suitable virtual joint prosthesis for use as a model for the actual endoprosthesis.
What treatment techniques are included in the range of services performed by knee endoprosthesis specialists?
In principle, surgeons try to replace only as much of the knee joint surface as the disease makes necessary. This means that they use a smaller or larger partial endoprosthesis (sled prosthesis) suitable for the degree of cartilage and bone degradation or even a knee TEP (stage-adapted knee prostheses).
As well as selecting the right type of prosthesis, the range of services performed by a knee endoprosthesis specialist includes the following techniques:
- use of resurfacing prostheses (mini-prostheses) as temporary prostheses in the case of limited cartilage damage
- use of sled prostheses, i.e. replacement of the inner-side or outer-side knee joint half
- replacement of the femoropatellar joint (joint between the thigh bone (femur) and knee cap (patella))
- use of total endoprostheses (TEP) - surface replacement of worn joint surfaces, i.e. the whole knee joint surface is replaced
- use of axis-guided knee prostheses in the case of advanced gonarthrosis and to correct leg axis malpositions (knock knees, bow legs) or to treat joint instability (loose knee joint)
- replacement of a damaged patella back surface
- production of special prostheses for certain patient groups (for example, people with allergies)
- performance of revision endoprosthesis operations (surgery to replace endoprostheses)
What are the special features of knee endoprosthesis specialists?
Knee endoprosthesis experts are generally doctors specializing in orthopedics and accident surgery, who have many years of experience, especially in the field of knee endoprosthetics. They can reliably diagnose arthrosis of the knee joint and other disorders and can then choose the most suitable therapeutic technique for the patient. They also have certificates (country-specific) in support of the high quality of their surgical care.
References
- Lützner J, Schmitt J, Lange T et al. (2016) Knietotalendoprothese: Wann ist der Ersatz angebracht? Dtsch Arztebl 113(44): A-1983 / B-1664 / C-1649
- Grifka J, Krämer Orthopädie J (2013) Orthopädie Unfallchirurgie. Springer, Heidelberg
- Michael JWP, Schlüter-Brust KU, Eysel P (2010) Epidemiologie, Ätiologie, Diagnostik und Therapie der Gonarthrose. Dtsch Arztebl Int 107(9): 152-62. doi: 10.3238/arztebl.2010.0152