The ovaries are connected to the uterus via the fallopian tubes. They are attached via ligaments and are thus held in position. As with the uterus, fallopian tubes, and vagina, the ovaries are part of the internal female reproductive organs.
The essential functions of the ovaries include the secretion of the female sex hormones:
- Estrogen,
- Progestogen, and
- Androgen.
These hormones are responsible for maintaining the menstrual cycle. In addition, the ovaries produce ova, which are released into the fallopian tubes during ovulation. From there, the egg cells migrate to the uterus. If they are fertilized by a sperm during this period, they develop into a fetus and the woman is pregnant.
The ovaries change their location and size during the menstrual cycle. However, they have a relatively large amount of space in the abdominal cavity. Therefore, their increase in size and change in location during the cycle does not affect other organs.
That’s why ovarian tumors often remain unnoticed for so long. Most often, they do not cause symptoms until they reach an advanced stage.
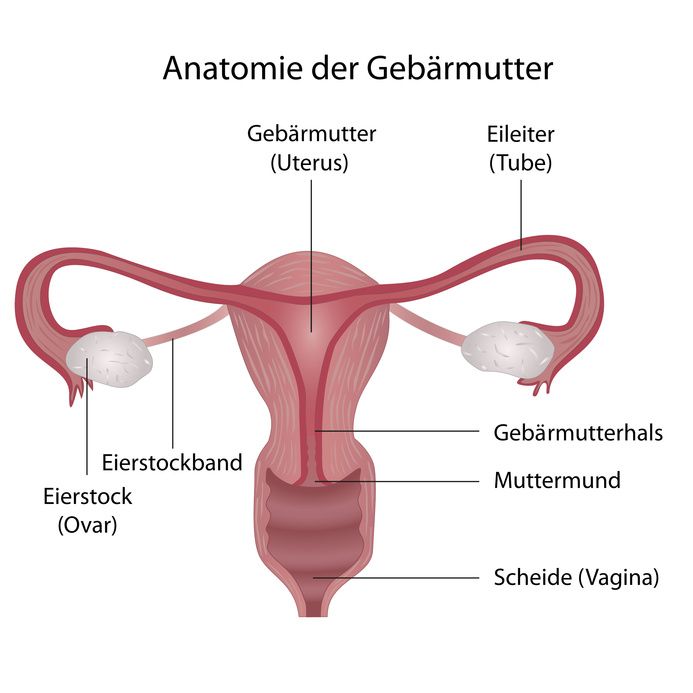
The ovaries, uterus, and vagina are internal sexual organs of women © bilderzwerg | AdobeStock
The exact cause of ovarian cancer has not yet been clarified. However, there are some known risk factors that can increase the likelihood of developing ovarian cancer. These include
- An older age,
- Harmful environmental influences,
- Unhealthy eating habits,
- Being overweight,
- Childlessness and infertility, and
- The use of hormone medications after menopause, among others.
In addition, genetic causes appear to be responsible for about 10 percent of all ovarian cancer cases. In these cases, mutations of the so-called breast cancer genes BRCA1 (on the 17th chromosome) and BRCA2 (on the 13th chromosome) are present. These genes also increase the risk of developing breast cancer.
If mutations of these genes are present, cases of ovarian cancer and breast cancer occur more frequently within a family.
Ovarian cancer is the second most common cancer of the female reproductive organs after breast cancer.
According to the Robert Koch Institute, between 7,000 and 8,000 women are newly diagnosed with ovarian cancer in Germany every year. This corresponds to an incidence rate of 11 new cases per 100,000 women annually.
Overall, the risk of developing ovarian cancer at some point in their lives is 1.5 percent for women. Older, postmenopausal women are most affected.
In about 50 percent of ovarian cancer cases, both ovaries are affected by malignant tumors.
In about 70 percent of cases, ovarian cancer is not discovered until the disease is well advanced. This is partly because ovarian cancer usually does not cause early symptoms in the beginning.
The symptoms, which mostly only appear at an advanced stage, are also rather nonspecific, meaning they can also be the result of many other, harmless diseases. What is more, there are no reliable screening tests for ovarian cancer to date.
Nonspecific symptoms that may occur in the advanced stages of ovarian cancer include
- Pain in the lower abdomen,
- Frequent urination, and
- Gastrointestinal complaints, e.g.,
In addition, affected women often feel tired, exhausted, and listless. Other possible symptoms are
- Bleeding outside of menstruation or after menopause,
- Unclear weight loss, and
An increase in abdominal girth without weight gain, caused by an increased accumulation of fluid in the abdomen (ascites).
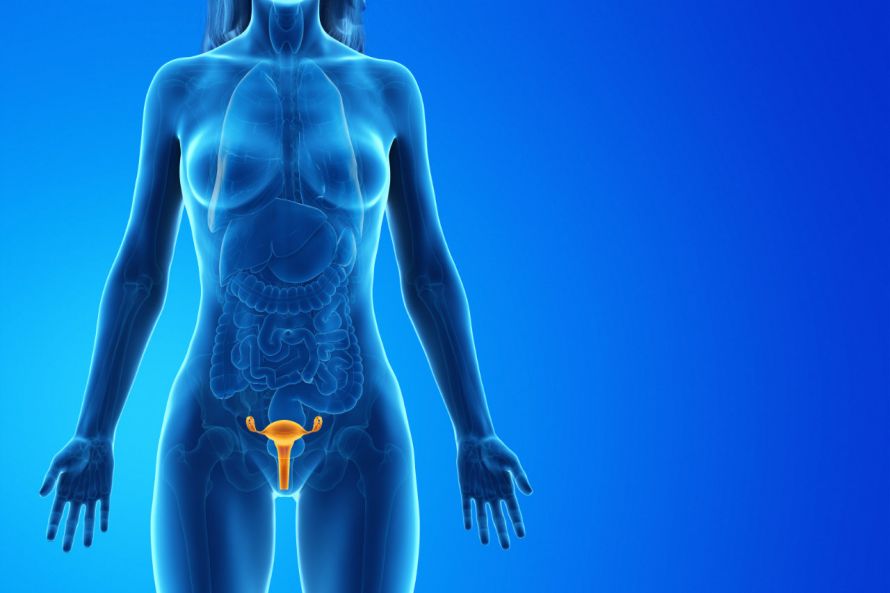
The location of the uterus and ovaries in the body © SciePro | AdobeStock
Ovarian cancer is staged according to what is known as the FIGO classification system (International Federation of Gynecology and Obstetrics). A distinction is made between four tumor stages:
- FIGO I: Ovarian cancer is completely limited to ovarian tissue. Only one ovary or both ovaries may be affected.
- FIGO II: Ovarian cancer has already spread to the pelvis.
- FIGO III: The ovarian tumor has already metastasized to the peritoneum or the lymph nodes.
- FIGO IV: The tumor tissue is already located outside the abdominal cavity, for example, as distant metastases.
The suspected diagnosis of "ovarian cancer" is usually made after nonspecific symptoms are reported if a gynecological examination is also performed as part of the diagnosis.
If ovarian cancer is suspected, the physician will perform further medical examinations to assess
- The size,
- Extent of spread,
- Location, and
- Texture
of the ovarian tumor. These can include, among other things, an ultrasound examination of the abdominal region (abdominal ultrasound) and the vagina (vaginal ultrasound). A CT scan is also possible.
However, the final diagnosis can only be made following surgery, during which the tumor tissue is removed. The tissue is then examined by a pathologist under a microscope for malignant cancer cells.
Treatment of ovarian cancer is provided by gynecologists specializing in gynecological oncology.
Surgery and chemotherapy are the two main therapeutic methods available for treating ovarian cancer and the choice of method depends on the stage of the disease. In most cases, however, treatment consists of a combination of both procedures.
Therefore, the tumor is first removed as completely as possible during surgery. As a rule, the following are removed
- Both ovaries,
- The uterus,
- The fallopian tubes,
- Part of the peritoneum,
- The appendix, and
- Lymph nodes in the pelvis and along the abdominal aorta
It is often necessary to supplement surgical treatment with chemotherapy, even if all parts of the tumor have been removed.
In advanced ovarian cancer, chemotherapy is often supplemented by an antibody therapy employing the active ingredient bevacizumab. Antibody therapy is designed to prevent the remaining cancer cells from forming new blood vessels. Even tumors need a blood supply.
After ovarian cancer treatment, regular follow-up examinations are important. They are used to detect a possible recurrence of ovarian cancer as early as possible.
These follow-up examinations should take place
- On a quarterly-basis for the first three years following completion of therapy,
- On a semi-annual basis in the subsequent two years, and
- On an annual basis thereafter.
The follow-up examination usually includes palpation of the abdomen and reproductive organs and an ultrasound examination of the abdominal and pelvic organs. In addition, the doctor asks questions about possible symptoms. Whether determining the levels of a tumor marker is appropriate must be decided on an individual basis.






















