Spondylosis is a collective term for several wear and tear diseases of the spine. This includes
- arthrosis of the spine,
- spondylarthrosis or
- the facet syndrome.
Typical of spondylosis is additional bone growth in particularly stressed areas of the spine – known as spondylophytes. Spondylosis can affect any part of the spine, i.e. the cervical spine, thoracic spine or lumbar spine.
With back pain, the reasons often lie directly in the spine © CLIPAREA.com / Fotolia
The International Classification of Diseases (ICD-10) lists spondylosis under the code M47. It is divided into five forms based on the clinical picture.
The type of spinal damage determines the category of spondylosis:
- Anterior spinal artery compression syndrome and vertebral artery compression syndrome: The deformed spinal column exerts pressure on the corresponding blood vessel exerts. When the nerve cells of the spinal cord do not receive sufficient nutrients and oxygen as a result, they suffer damage and die. Doctors call this damage to the spinal cord myelopathy.
- Spondylogenic compression of the spinal cord: The changes in the spine directly affect the spinal cord. The result is spinal canal stenosis.
- Spondylosis with radiculopathy: The spondylosis damages the nerve root here. Radiculopathy is also known as root syndrome for this reason.
There are also other spondyloses without myelopathy or radiculopathy. Here there are no neurological symptoms or discomfort.
The spine is subjected to a lot of stress in the course of a person's life. With increasing age, the flexibility of the intervertebral discs between the vertebral bodies decreases. The intervertebral discs serve as a buffer for the vertebral bodies.
This allows superimposed vortices to approach and even touch each other. The so-called facet joints of the spine are affected first. This gives rise to the facet syndrome. You can see in the video how this wear and tear disease develops:
The wear and tear on the spine causes it to lose stability. Additional bone growth should re-strengthen and stabilise the spine. The body therefore forms spondylophytes, i.e. small bone spurs.
At the same time, this additional bone mass takes up more space. Under certain circumstances, the spondylophytes can press on the
- Nerves,
- Blood vessels and
- the spinal canal
drücken. Pain and neurological discomfort are the result.
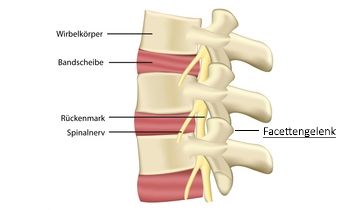
The vertebral bodies touch at the facet joints – in spondylosis, the bony contact surfaces increase © bilderzwerg / Fotolia
In some cases, the spondylophytes that grow on different vertebrae join together. This creates a cohesive bony structure that restricts the mobility of the spine. When the spine is deformed in this way, doctors speak of spondylosis deformans.
In addition, there are special forms that arise differently. Spondylosis hyperostotica, for example, is due to a metabolic disorder. A potential cause of spondylosis hyperostotica is diabetes.
Depending on which areas of the vertebrae are affected by spondylosis, different symptoms occur. The signs of wear and tear typically first manifest themselves with mild symptoms and pain. More severe complaints only appear gradually.
Back pain is common with spondylosis. The pain may also occur in the neck or radiate to the arms and legs.
Spondylosis affects the spinal cord and peripheral nerves to some extent. If the spinal nerves or spinal cord are damaged, other neurological symptoms typically occur:
- Sensory disturbances, for example tingling in the arm
- Loss of control over bladder and bowel
- Numbness
- Unexpected weakness that is not explained by the muscles
- Movement disorders, e.g. gait disorders, and paralysis
In many adults, the first signs of wear and tear on the spine and intervertebral discs become apparent at an early age. They progress with age.
The overwhelming majority of people over the age of 65 have bone spurs on their vertebrae. But only a portion of those affected suffer from
- Back pain,
- Movement restrictions or
- other symptoms.
Spondylosis often remains undetected and asymptomatic.
Spondylosis sometimes leads to other problems. Spondyloses with radiculopathy or myelopathy burden the patient with neurological symptoms and nerve pain. In the course of the disease, muscle tension is also possible, which causes pain.
The muscle tension often arises because of a protective posture that sufferers adopt due to spondylosis.
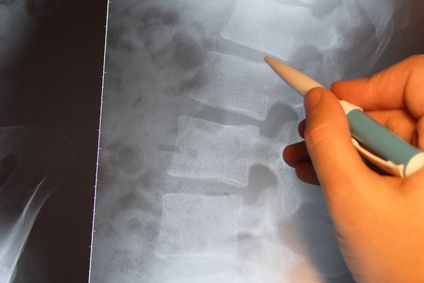
The X-ray shows changes in the spine © luxpainter / Fotolia
A doctor usually carries out
on which the condition of the spine can be seen. In this way, other possible diseases can also be ruled out.
Further tests may be required, for example to check for any nerve deficits. The doctor often also takes a blood sample to rule out inflammation as a cause.
An operation can relieve the spinal cord, which may be at risk, or help to make the spine more mobile again. A doctor will only consider surgery if other treatment options have already been exhausted or do not seem sufficient in the individual case. The exact procedure is different for each patient.
If the cause of the pain is facet syndrome, injections prove to be an effective pain therapy. The video shows how a facet infiltration works:
In some cases, the surgeon removes the offending spondylophytes and widens the spinal canal. This is how he fixes the nerve compressions. The surgeon can also replace the vertebra with a prosthesis.
In other cases, the doctor only corrects the position of the vertebra. The videos inform you about the surgical options:
Sometimes spondylosis can be traced back to diabetes or another metabolic disorder. Then the treatment of this underlying disease plays an important role.
Often, if you have spondylosis, you will be given painkillers to relieve the symptoms.
The best time for preventive measures is when you do not yet suffer from spondylosis. Typical signs of ageing, such as fatigue of the intervertebral discs, cannot be completely prevented. Nevertheless, something can be done for back health.
This way you can reduce the risk of spondylosis:
- Strengthen your muscles – make sure to train your back and abdomen evenly to avoid imbalances. These put strain on the spine due to unbalanced stability and different tensile forces.
- Don't forget to stretch! Strong and supple muscles naturally support the body.
- Make sure you have a healthy posture – when sitting or standing, but also when carrying heavy objects.
- An ergonomically designed desk also helps to maintain back health for longer.
- A healthy body weight means relief for the spine and joints.
If your back pain does not improve over three to six weeks, consult a doctor.
In many cases, a physiotherapist helps patients improve their back health. The physiotherapist takes into account the specifics of the disease. Not every type of sport is suitable for training the back muscles in spondylosis.
Jerky movements, for example, are generally considered problematic for back problems.

Physiotherapy often helps with progressive spondylosis © drubig-photo / Fotolia
Most older people have bone spurs on their vertebrae. With these spondylophytes, the body tries to strengthen the degenerating spine. Herniated discs and metabolic diseases are among the risk factors.
After an inconspicuous initial period, spondylosis sometimes develops into a serious problem. Pain and muscle tension affect the quality of life and the spinal cord may be at risk.
Therefore remember to take preventive measures and have a consultation with your doctor at an early stage, so that you promote your back health.



















































