Here you can find additional information and selected specialists and centers for the treatment of esophageal cancer.
Here you can find additional information and selected specialists and centers for the treatment of esophageal cancer.
Recommended specialists
Brief overview:
- Anatomy: Food passes from the mouth into the stomach via the approximately 25 cm long esophagus.
- What is esophageal cancer? A malignant tumor disease of the esophagus.
- Symptoms: Symptoms do not appear until the later stages of the disease. Swallowing difficulties and pain behind the sternum or in the upper abdomen then occur. Unwanted weight loss, vomiting, increased salivation, and other symptoms may also occur.
- Risk factors: Smoking, increased consumption of high-proof alcohol, and an unbalanced diet. There are numerous other risk factors and precancerous conditions that increase the likelihood of a tumor developing in the esophagus.
- Diagnosis: If suspected, an esophagoscopy is conducted, which allows the doctor to view the inside of the esophagus. The size and spread of the tumor are determined by an endoscopic ultrasound, CT scan, ultrasound of the liver, and other diagnostic tests.
- Treatment: Surgery is the most important treatment procedure. Often, this involves removing all or part of the esophagus. If necessary, chemotherapy or chemotherapy in combination with radiotherapy may be administered beforehand (combined radiation chemotherapy).
- Prognosis: Since the tumor is often discovered late, the prognosis is rather unfavorable; on average, 21% of patients are still alive after five years.
Article overview
What is the esophagus?
The esophagus is a muscular tube about 25 centimeters long. It is the connection between the mouth or pharynx and the stomach. The esophagus has a diameter of about two centimeters.
It transports chewed food from the mouth to the stomach by means of undulating movements. Sphincters at the upper and lower ends close the esophagus. These sphincters open for the onward transport of food as needed.
The esophagus is divided into three sections:
- Neck section (cervical area)
- Chest section (thoracic area)
- Esophagus-stomach junction (gastro-esophageal junction)
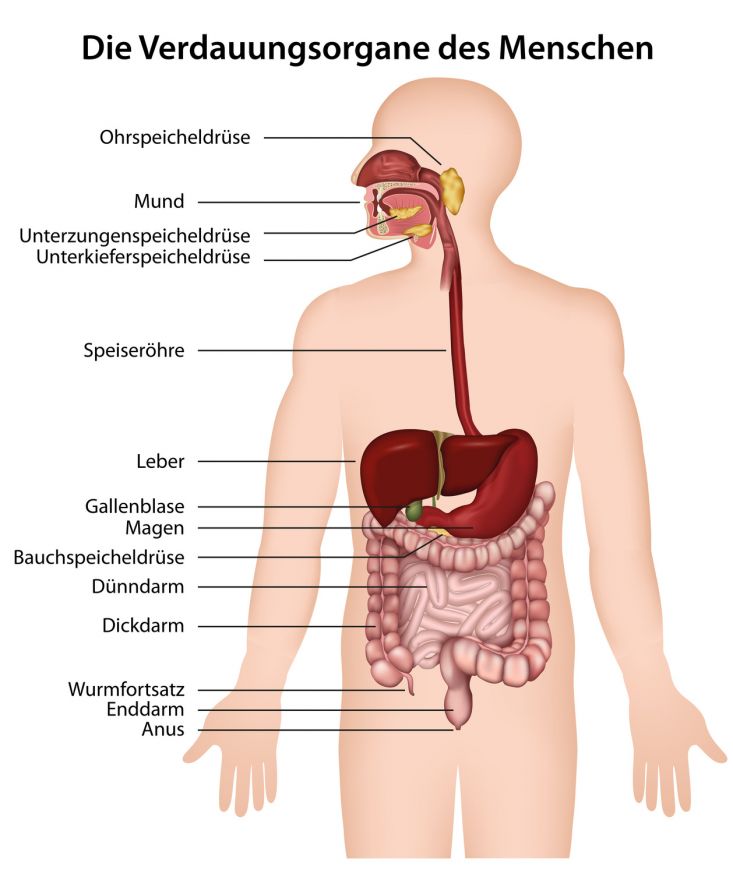
The esophagus is the tube connecting the throat and the stomach © bilderzwerg / Fotolia
The interior of the esophagus is lined by a mucous membrane (mucosa), the uppermost layer of which consists of squamous cells. This is followed by a layer of
- Nerves,
- Blood vessels,
- Glands,
and then a muscle layer. A layer of connective tissue links the esophagus with other organs. At the junction with the stomach, the mucosa of the esophagus merges with the glandular-rich mucosa of the stomach.
Definition: What is esophageal cancer?
Esophageal cancer is a malignant cancer of the esophagus. In Germany, approximately 5,700 men and 1,700 women were newly diagnosed with esophageal cancer in 2018. The median age of onset was 67 years for men and 71 years for women in 2014.
The two most common and important types of esophageal cancer are squamous cell carcinoma and adenocarcinoma.
- Adenocarcinoma (Barrett's carcinoma) originates in the glandular tissue. It occurs almost exclusively at the junction with the stomach.
- Squamous cell carcinoma, on the other hand, originates from the mucosa.
Squamous cell carcinomas account for the largest proportion of esophageal cancer cases with 50 to 60 percent, while adenocarcinomas account for about one-third.
What are the symptoms of esophageal cancer?
The esophagus is a very elastic organ. Symptoms therefore only arise at a late stage. The tumor is then so large that it impairs the functionality of the organ. Esophageal cancer is therefore often referred to as "silent cancer."
A leading symptom of the later stages of the disease is dysphagia (difficulty swallowing). In this case, the swallowing process is impaired by the tumor taking up space. Patients perceive this as pain behind the breastbone or in the upper abdomen, accompanied by feelings of pressure.
For patients to have problems swallowing at all, the cancer must have already significantly narrowed the esophagus. The narrowing of the esophagus makes it difficult to eat. As a result, many patients can no longer eat solid foods and they lose several kilograms of body weight within a few weeks. In a large proportion of cases, esophageal cancer is therefore associated with unwanted weight loss.
Other symptoms include
- Vomiting,
- A lack of appetite, and
- Digestive disorders.
Around one third of those affected also complain of
- Regurgitation, i.e., vomiting food and
- An increased flow of saliva.
If the cancer occurs in the lower part of the esophagus, coughing may be a possible symptom. If the tumor also presses on the larynx or the vocal cords, hoarseness is also a factor.
In an advanced course and in the case of metastasis, enlarged lymph nodes in the neck area can be palpated.
Causes of esophageal cancer
It has not yet been clearly explained why tumors develop in the esophagus. However, there are certain factors that increase the risk of disease.
The most important risk factors for developing squamous cell carcinoma are
- Smoking,
- An increased consumption of high-proof alcohol,
- An unbalanced diet with a low proportion of fruit and vegetables, and
- The frequent consumption of very hot food and drinks.
Adenocarcinomas often develop as a result of a reflux disease. In this clinical picture, persistently acidic gastric juice flows into the esophagus and irritates the tissue there (chronic heartburn).
This chronic reflux of digestive fluids into the esophagus increases the likelihood of developing Barrett's esophagus, an inflammatory change with ulceration in the lower part of the esophagus where it joins the stomach (gastroesophageal junction).
Barrett's esophagus is a so-called precancerous condition that can develop into carcinoma. Therefore, adenocarcinoma is also known as Barrett's carcinoma. Other risk factors for the development of adenocarcinoma include
- Smoking,
- Not consuming enough fruit and vegetables, and
- Being overweight.
A large proportion of esophageal tumors develop from a precancerous lesion. Plummer-Vinson syndrome is also a precancerous condition from which an esophageal tumor may develop. The syndrome develops in people with prolonged iron deficiency anemia. It is characterized by, among other things, torn corners of the mouth and dysphagia.
Achalasia (a functional disorder of the esophagus) can also result in esophageal cancer in the long run. In esophageal achalasia, the function of the lower esophageal sphincter is impaired. Among other things, this allows undigested food from the stomach to flow back into the esophagus.
In addition to the risk factors mentioned above, other factors increase the likelihood of esophageal cancer developing:
- Scarring after alkali chemical burns and
- Prior radiotherapy in the esophageal area to treat other cancers.
It is uncertain whether human papillomavirus infections also have an influence.
Diagnosis of esophageal cancer
Pre-existing conditions and the presence of risk factors in combination with
- Difficulty swallowing,
- Hoarseness, or
- Coughing
can be considered the first indication of possible esophageal cancer.
However, to confirm the diagnosis, an endoscopy of the esophagus (esophagoscopy) must be performed. To do this, the doctor inserts a thin, tube-shaped, and flexible instrument with an integrated light source and camera (endoscope) into the esophagus via the mouth. This allows the physician to examine the surface of the esophagus for abnormal tissue changes.
For better detection of tissue changes, mucosal areas can be stained (chromoendoscopy) and evaluated by a computer. If suspicious areas are detected, the doctor can also immediately take a tissue sample. In the laboratory, a pathologist examines this sample histologically. This allows esophageal cancer to be identified unambiguously.
In order to initiate the appropriate therapy, the size and spread of the tumor must be determined. An endoscopic ultrasound can be used to assess
- How deep into the tissue the tumor has already grown and
- Whether it has spread to neighboring tissue.
A Computed tomography (CT) scan of the neck, chest, and abdomen and an ultrasound examination of the liver serve to diagnose the spread of the disease. This refers to the search for possible metastases and their spread to neighboring tissue.
In the case of advanced tumors,
- PET-CT scans (combination exam of a positron emission tomography and CT scan),
- Magnetic resonance imaging examinations (MRI) can be used as an alternative to CT, if necessary,
- Laparoscopies (abdominal endoscopy), and/or
- Thoracoscopies (endoscopy of the thoracic cavity and pleura)
may also be used to detect metastases. The results of these exams enable tumor staging using the TNM staging system, which allows the therapy with the most promising results to be selected.
Esophageal carcinoma therapy
Patients with esophageal cancer should be cared for by experienced experts at specialized centers.
Within the framework of an interdisciplinary tumor board, the best possible treatment for the patient will be discussed in detail with the participation of
- Radiologists,
- Gastroenterologists,
- Oncologists,
- Radiation oncologists, and
- additional special disciplines, if applicable.
The treatment methods that are used to treat esophageal cancer depend on
- The situation,
- The spread,
- The type, and
- The aggressiveness of the tumor.
Whether the tumor is localized or has already spread to neighboring tissues or other organs is therefore of great importance.
Surgery in the context of esophageal surgery, where the tumor is removed from the esophagus, is the decisive procedure. Prior to surgery, the patient often undergoes chemotherapy or combined radiation chemotherapy. These neoadjuvant treatment methods can increase the chances of success.
In the early stages of cancer, it is often sufficient to perform an endoscopy. In this procedure, the surgeon removes the upper portions of the esophageal mucosa with a snare. This is possible if the tumor is still confined to the esophageal mucosa (so-called early carcinoma). Under certain circumstances, the esophagus can be completely preserved in this way.
However, larger tumors usually require complete or at least partial removal of the esophagus. Depending on the patient's condition and the extent of the cancer, esophagectomies may be carried out
- in an open surgical technique,
- partially (so-called hybrid technology), or
- completely in a minimally invasive technique (keyhole surgery).
The use of minimally invasive esophageal surgery can significantly reduce the complication rates of esophageal cancer surgery. Studies have demonstrated the advantages of minimally invasive esophageal surgery for the patient. The hybrid technique or a completely minimally invasive procedure is therefore considered the new gold standard.
The remaining parts of the esophagus are then connected to the stomach. Thus, food intake is possible even after surgery. A portion of the stomach that is shaped into a gastric tube then acts as an esophageal substitute. This technique facilitates a very good swallowing function and thus achieves an improved quality of life.
If the stomach also needs to be partially or completely removed, part of the small intestine can be reshaped to form the esophagus.
To improve the prognosis, the lymph nodes in the abdomen and the thorax/mediastinum (so-called 2-field lymphadenectomy), and in some cases also in the neck (so-called 3-field lymphadenectomy) are removed.
If metastases have already formed in other organs, the operation does not serve to cure the disease, but rather to alleviate the symptoms. This is referred to as palliative therapy.
Esophageal cancer prognosis
The prognosis of esophageal cancer is rather unfavorable. Unfortunately, the tumor is often discovered late. In most patients, it has already metastasized by then. Only one in seven tumors is detected at an early stage.
Five years after diagnosis, only about 21 percent of patients are still alive.
What distinguishes esophageal cancer specialists?
Patients with esophageal cancer should seek treatment at hospitals with special expertise in this area. There, various esophageal cancer experts work together in a tumor conference. Together they develop an individual treatment strategy for the patient.
Predominantly specialists from the fields of
- Gastroenterology,
- Oncology,
- Radiotherapy,
- Radiology,
- Surgery, and
- Pathology
meet. These experts take into account the diagnostic and therapeutic procedures recommended by guidelines.
Oncology treatment centers, which are generally certified by the German Cancer Society, ensure a permanently high quality of care for patients with esophageal cancer.






















